Brain & Neurovascular Surgeries
- Brain & Neurovascular Surgeries
- Brain Tumor SurgeryBrain Tumor Surgery
- Skull Base Tumor SurgerySkull Base Tumor Surgery
- Neurovascular SurgeryNeurovascular Surgery
- Endovascular NeurosurgeryEndovascular Neurosurgery
- Stroke Surgery & ThrombectomyStroke Surgery & Thrombectomy
- Traumatic Brain Injury SurgeryTraumatic Brain Injury Surgery
- Pituitary Tumor SurgeryPituitary Tumor Surgery
- Hydrocephalus Surgery Hydrocephalus Surgery
- Epilepsy SurgeryEpilepsy Surgery
- Functional NeurosurgeryFunctional Neurosurgery
Hydrocephalus Surgery (VP Shunt / ETV)
Hydrocephalus is a condition in which cerebrospinal fluid (CSF) accumulates abnormally in the brain’s ventricles, leading to increased intracranial pressure. This can cause symptoms such as headache, vomiting, blurred vision, imbalance, and in infants, an enlarged head. Surgical intervention is the mainstay of treatment to restore normal CSF flow and relieve pressure on the brain.
1- Ventriculoperitoneal (VP) Shunt
ProcedureA VP shunt involves placing a flexible tube (catheter) system inside one of the brain’s ventricles. The shunt diverts excess CSF from the brain to the peritoneal cavity (abdomen), where it is absorbed into the bloodstream.
Components of the VP Shunt System:- Ventricular catheter: Inserted into a brain ventricle.
- Valve mechanism: Controls the flow and pressure of CSF.
- Distal catheter: Carries CSF from the valve to the abdomen.
- Obstructive (non-communicating) hydrocephalus.
- Communicating hydrocephalus due to meningitis, hemorrhage, or trauma.
- Normal pressure hydrocephalus in adults.
- Can manage most types of hydrocephalus.
- Provides continuous drainage and pressure regulation.
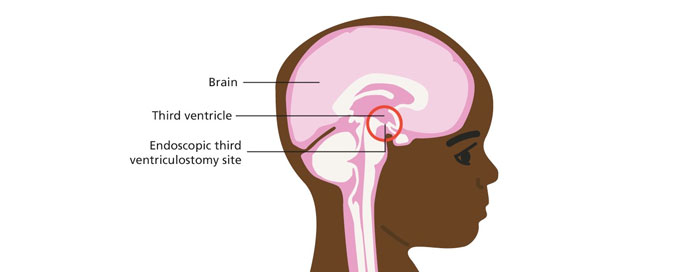
2- Endoscopic Third Ventriculostomy (ETV)
ProcedureETV is a minimally invasive procedure performed using a neuroendoscope. The surgeon makes a small hole in the floor of the third ventricle, allowing CSF to flow directly from the ventricles into the basal cisterns, bypassing any obstruction in the ventricular pathways.
Indications- Obstructive hydrocephalus caused by aqueductal stenosis, tumors, or cysts.
- Cases where shunt independence is desirable.
Advantages
- No foreign body (shunt) implantation.
- Lower risk of infection.
- Long-term independence from shunt system.
Limitations
- Not suitable for all types of hydrocephalus (especially communicating types).
- Risk of closure of the opening over time, requiring reoperation.
3- Postoperative Care
- Monitoring for symptoms of shunt blockage or infection (fever, headache, vomiting, altered consciousness).
- Regular imaging (CT/MRI) to assess ventricle size and CSF flow.
- Lifelong follow-up for shunt-dependent patients.
- In ETV cases, endoscopic review may be required if symptoms recur.
